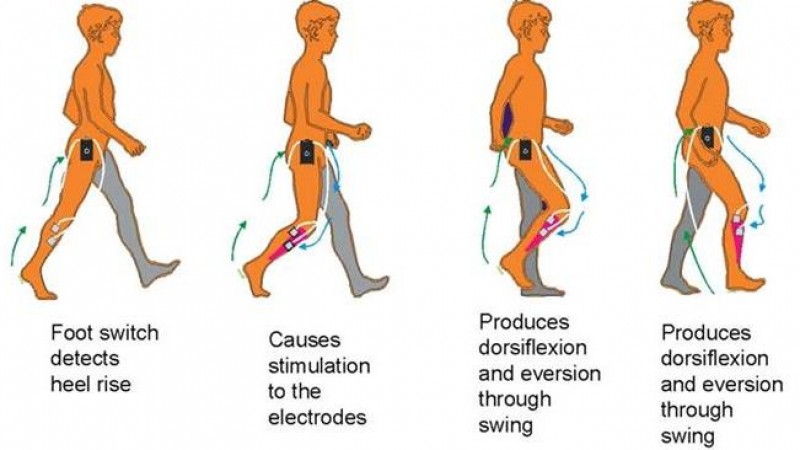
Foot drop is a temporary or permanent muscular weakness or paralysis that affects people’s ability to lift the front part of the foot and move their toes. It is caused by neurological problems where signals from the brain can no longer control movements, such as walking or grasping. Often a sympton of a greater health problem, the condition may cause pain in the foot and ankle or imbalance when walking.
FES is a method of externally and electrically controlling muscles to generate movement. Foot drop stimulators are one type of FES method which is used to improve symptoms of a number of conditions such as spinal cord injuries, strokes or multiple sclerosis. Drop foot stimulators are used to activate nerves, resulting in the contraction of muscles which are used in walking, for example. During FES assisted walking, just before a patient lifts their heel, mild electricity stimulates the peroneal nerve which supplies movement to the lower leg, foot and toes. This results in contraction of the muscles responsible for moving the foot into an ordinary upwards position, enabling a smooth walking movement.
The impact
Professor Ian Swain’s BU research, in collaboration with Salisbury NHS Foundation Trust, has particularly focused on FES treatment for foot drop. This informed treatment has contributed to the care of over 7,000 patients in Sailsbury.
Odstock Medical Limited (OML) was established by the Salisbury NHS Trust in 2006. The business was the first NHS company to be set up in England. The reason for launching the corporation was to use commercial management to maximise income from developed FES products which could be filtered back into research and development, while creating an income for the NHS Trust. This has allowed money to be spent on developing new products while already developed FES systems are sold more widely.
The partner group, consisting of BU, OML and the NHS, have worked with universities such as Surrey, Southampton, Salford and University College London (UCL). Together, collaboration has achieved a number of firsts, such as the first implanted foot drop stimulator clinical service in the world, the National Clinical FES Centre in Salisbury.
Since 2014, OML has trained more than 600 staff, both in the UK and overseas, and seen great commercial success. BU research innovation has created cost-effective FES devices, which have sold by more than 20,000 units worldwide.
The difference FES makes to the lives of individuals is evidenced by testimonials on OML’s website:
“I have been using a single-channel stimulator for foot drop, due to MS, for five years. I wear it every day and it has allowed me to carry on working full-time. It is the single most helpful thing in this journey as a patient, and has allowed me to remain as active as possible.”
Recent research
In recent years, Professor Swain’s FES research has expanded into areas other than neurorehabilitation. He has now published papers on the use of stimulation to reduce swelling and improve blood flow in the lower leg; and on the safety implications of using electrical stimulation for a person with a pacemaker or implanted defibrillator.
Work at the National Clinical FES Centre has also explored the use of electrical stimulation to improve constipation in people with neurological problems such as MS, PD and SCI. Continued investigation with OML has now led to the development of a musculosketal stimulator aimed at the orthopaedic market, currently going through commercialisation processes. The team have also collaborated with Loughborough University in using FES to improve recovery and prevent further injury in people with severe ankle sprains.
Work continues to grow in FES research, thanks to a number of PhD studies. For example, BU PhD student Varshini Nandakumar is investigating adaptive walking FES systems for people with neurological problems. The aim is to create a system which is able to detect changes in terrain, such as slopes or curbs. Another BU PhD student, Nathan Barretthas, recently submitted his PhD thesis on the use of FES and computer games in improving hand and arm function after a stroke.
The future
Professor Swain’s research is now focused on improving upper limb function, and making systems more intelligent and easier to use by employing wireless technology. In five years, the project aims to distribute a new range of FES devices. Areas of electric stimulation development for application are Parkinson’s Disease, constipation and rehabilitation after stroke, hip and knee replacement surgery.
OML aspire to have FES as a routine treatment throughout the NHS, including within District General Hospitals in the UK, and in developing overseas markets. In 2009, the National Institute for Health and Care Excellence (NICE), who provide national guidance and advice to improve health and social care, approved the use of BU developed FES for foot drop.
OML now plans to upgrade existing equipment by devising new products and techniques, again informed by research, which can be distributed to clinical centres worldwide.
A significant expansion of research at BU has been in Professor Swain’s recent move to the Orthopaedic Research Institute (ORI). This move aims to expand current rehabilitation techniques for people with neurological problems to assist those recovering from orthopaedic issues such as joint replacement surgery.
Finally, a grant of £157,000 has just been obtained for the wellbeing charity INSPIRE to develop a practical stimulation system for people with tetraplegia in order to improve their hand function. The project will be led by Dr Vinil Chackochan of the Faculty of Science and Technology. It is intended that a practical device, suitable for the open market, will be developed for use at home by the project’s end.
 Professor Ian Swain
Professor Ian Swain